
What Is A Carotid Endarterectomy?
Carotid endarterectomy is a surgical procedure performed to remove plaque buildup inside the carotid artery, so that normal blood flow may be restored. This procedure is usually recommended for patients who have suffered from a transient ischemic attack (TIA), stroke, and whose carotid arteries are at least 70 percent blocked.
Carotid Endarterectomy Procedure
After the patient has received general anesthesia, a carotid endarterectomy will begin with an incision made in the neck to expose the narrowed carotid artery. A shunt is put in place to direct blood flow away from the area being operated on. The surgeon opens the artery and removes the plaque, usually in one piece. A vein from the leg may be grafted onto the carotid artery in order to widen it. The shunt is removed and all incisions are closed. The carotid endarterectomy procedure usually takes two hours.
Recovery After Carotid Endarterectomy
Day-to-day activities can be continued about a week after surgery, as long as they don’t involve strenuous physical labor. Neck aches may last for about 2 weeks after surgery so it is important that the patient not turn their head too fast during the recovery period.
Risks Of Carotid Endarterectomy
As with any surgical procedure, there are risks associated with the carotid endarterectomy procedure. Some of these risks include a reaction to anesthesia, the development of blood clots, a heart attack, stroke, redevelopment of plaque buildup, infection, and death.
What Is An AV Fistulas?
The artery-to-vein (arteriovenous, or AV) connection can be created in one of two ways: with a graft or with a fistula. A graft is an artificial tube; an AV fistula is a direct surgical connection of one vessel to the other using the patient’s own tissues. Although fistulas typically take three to six months to mature, while grafts only take two to six weeks, doctors prefer to use fistulas because they tend to be stronger than grafts and have a lower risk of infection.
How Are AV Fistulas Treated?
Grafts may be recommended for patients with small, blocked, or scarred veins. If the patient needs immediate treatment, a tube called a venous catheter may be used for a few weeks or months until the fistula or graft is ready.
Central Venous Catheters
Central venous catheters are hollow tubes used for the efficient delivery of chemotherapy drugs, fluids, blood or other medications, or for regular blood sampling, over the course of a few weeks or months. One end of the catheter is placed in the largest vein in the chest, called the Superior Vena Cava or SVC. The other end may be tunneled just beneath the skin’s surface or surgically implanted as a port, short for portacath. Catheters called PICCs, or peripherally inserted central venous catheters, may be inserted by a peripheral blood vessel.
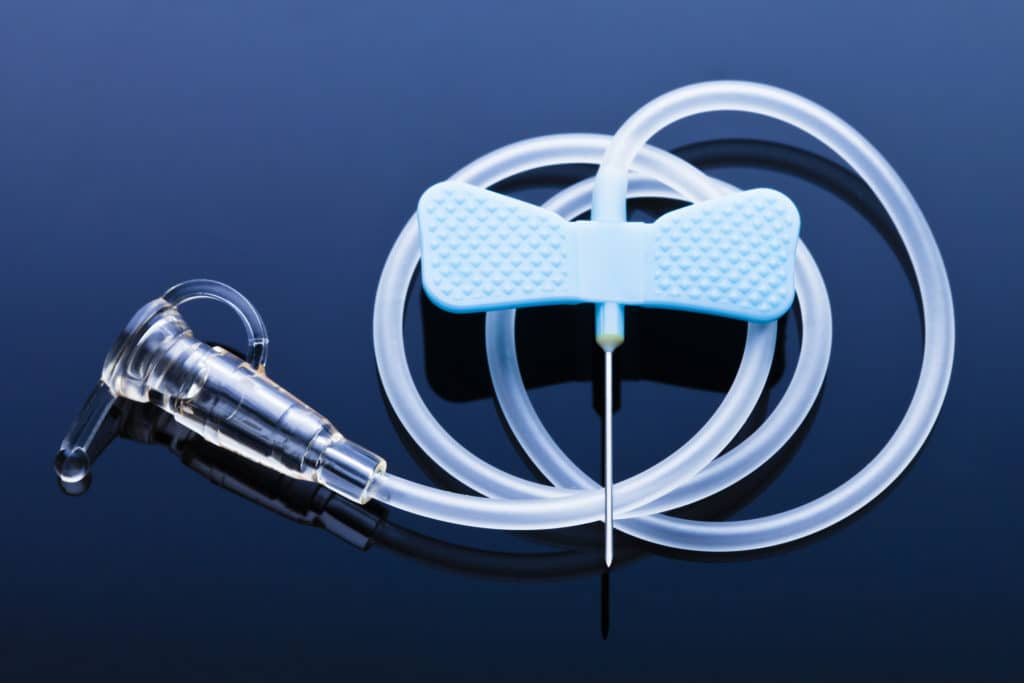
Dialysis Access
What Is A Catheter?
Catheters are thin tubes designed to be inserted into the skin to provide an easy method for conveying fluids, or sometimes gases, through the body. Catheters can be inserted into a variety of body cavities, ducts, and blood vessels, allowing the passage of nutrients, blood, or medications. They substitute for intravenous lines when vascular assistance is needed for a longer period of time. In the case of dialysis for kidney disease, blood with waste products flows through the catheter. In the case of chemotherapy, medication is conveyed. In both cases, catheters take over the job of the usual blood vessels. When a catheter is installed for long-term use it is called a permcath.
Uses Of Catheters
Catheters are used for many purposes before, during, and after surgery. These purposes may include:
- Intravenous antibiotic treatment
- Chemotherapy
- Nutritional support
- Repeated drawing of blood samples
- Hemodialysis
- Blood transfusions
Dialysis Procedure
Short for hemodialysis, dialysis is the most common treatment for chronic kidney failure. When the kidneys fail, they can no longer filter waste from the blood. Dialysis does the kidneys’ job for them: removing blood from a vein in the patient’s arm or leg, circulating it through a filtering machine, and returning it to the body through an artery.
Because veins tend to have weak blood flow, doctors often connect one of the patient’s nearby arteries to the vein being accessed for dialysis. This increases blood flow and strengthens the vein, which in turn allows more blood to flow. The vein’s increased strength and capacity help create a durable access site and provide ample blood flow for patients undergoing long-term dialysis.
The artery-to-vein also called arteriovenous, or AV, the connection can be created in one of two ways: with a graft or with a fistula.

A graft is an artificial tube; an AV fistula is a direct surgical connection of one vessel to the other using the patient’s own tissues. Although fistulas typically take three to six months to mature while grafts only take two to six weeks, doctors prefer to use fistulas because they tend to be stronger than grafts and have a lower risk of infection. Grafts may be recommended for patients with small, blocked, or scarred veins. If the patient needs immediate treatment, a tube called a venous catheter may be used for a few weeks or months until the fistula or graft is ready.
See What Our Patients Have To Say
"The doctors and staff were very friendly and professional. I feel very confident in there hands."
"I feel like I am I good hands. The staff was so family and made me feel like family. So glad I found this practice."
Schedule A Consultation!
If you are looking for more information and would like to schedule a consultation, call us today at (855) 803-6482 or fill out an online contact form and we will get back to you as soon as we can.

Monday – Thursday: 9am – 5pm
Friday: 9am – 1pm
Saturday – Sunday: Closed